Drug-induced Gingival Hyperplasia and Its Management a Literature Review
Continuing Education Activity
Drug-induced gingival overgrowth (DIGO), also referred to as drug-induced gingival enlargement, and previously known equally drug-induced gingival hyperplasia, is a noted side-event of certain drugs given for non-dental uses where the gingival tissue is not the intended target organ. The key offending drug classes are anticonvulsants, immunosuppressants and calcium aqueduct blockers. This action presents the causes, pathophysiology, and diagnosis of gingival overgrowth and highlights the role of the interprofessional squad in its direction.
Objectives:
-
Place the types of drugs associated with gingival overgrowth.
-
Review the pathophysiology of drug-induced gingival overgrowth.
-
Summarize the handling and management options available for gingival overgrowth.
-
Describe some interprofessional team strategies for improving intendance coordination and outcomes in patients with gingival overgrowth.
Access free multiple pick questions on this topic.
Introduction
Drug-induced gingival overgrowth (DIGO), likewise referred to as drug-induced gingival enlargement, and previously known every bit drug-induced gingival hyperplasia, is a side-event of certain drugs where the gingival tissue is non the intended target organ. The key offending drug classes are anticonvulsants, immunosuppressants, and calcium aqueduct blockers.[1] Gingival overgrowth impedes proper dental hygiene and, apart from the corrective damage, causes painful chewing and eating.
A not-surgical approach is the first line of treatment, including appropriate plaque control and discontinuing or changing the inducing drug. In the recent years azythromicin has gained a lot of attention due to its capacity to better gingival overgrowths in patients taking cyclosporin A, avoiding the need of changing the drug to another agent. Surgical direction comes in play but when medical treatment is unsuccessful, yet, recurrences are common and the results last for usually twelve months.[two]
Etiology
Drugs are the most common reason backside gingival enlargements. DIGO is a side effect seen in patients taking anticonvulsants, immunosuppressants, or calcium channel blockers. It is associated with the patient'due south genetic predisposition and the presence of existing plaque or gingival inflammation.[iii]
Anticonvulsants
Phenytoin (PHT, or 5,5-diphenylhydantoin), sodium valproate, phenobarbitone, vigabatrin, primidone, mephenytoin, and ethosuximide are some of the drugs that crusade gingival hypertrophy. All the same, phenytoin is the anticonvulsant most associated with gingival enlargements.[4] It is used to treat temporal lobe, tonic-clonic, and psychomotor seizures.[4]
Drugs similar PHT, phenobarbitone, and primidone are metabolized to 5-(4-hydroxyphenyl) v-phenyl hydantoin (4-HPPH), responsible for overgrowth gingival tissue.
At times, multiple anticonvulsants are given together, acting synergistically and aggravating the condition.
Immunosuppressants
Immunosuppressants are prescribed after organ transplantation to prevent organ transplant rejection, such every bit renal transplants, and treat some autoimmune diseases, like rheumatoid arthritis.[four]
Cyclosporin, sirolimus, and tacrolimus are immunosuppressants linked to gingival enlargement. Cyclosporin is the most oftentimes prescribed immunosuppressive drug after an organ transplant, and the incidence of gingival overgrowth has been constitute in about 53% of patients taking cyclosporin later renal transplants.[5] Tacrolimus, on the other hand, is less toxic than cyclosporin, causing less astringent gingival overgrowth, hepatic and renal toxicity.[6][7][6] Sirolimus is another immunosuppressant that has shown a predisposition to gingival enlargement.[8][9][10][eight]
Calcium Channel Blocker
Calcium channel blockers are indicated for treating hypertension, angina pectoris, and peripheral vascular disease.[four] These include nifedipine, nitrendipine, felodipine, amlodipine, nisoldipine, verapamil, and diltiazem. Seymour et al. reported the first case of gingival overgrowth attributed to amlodipine in 1994. Lafzi et al. reported gingival hypertrophy in patients receiving ten mg of amlodipine daily within ii months of the onset of handling.[11]
Renal transplant patients taking immunosuppressants like cyclosporin show a greater propensity to develop gingival hypertrophy when put on nifedipine or diltiazem. Nevertheless, the extent of hypertrophy is more than pregnant with cyclosporin.[4] Combinations of these drugs could act synergistically, causing exaggerated hypertrophy of gingival tissue.
Epidemiology
Drug-induced gingival overgrowth is about unremarkably seen in male children and adolescents, with a most prevalent location in the anterior gingival tissue. The genotype of the individual have an outcome on the evolution of DIGO,[12] and the extent and degree of overgrowth depend on the drug. Phenytoin, cyclosporin, and nifedipine are the most mutual causes of gingival overgrowth, and phenytoin has the highest prevalence of all. It is estimated that 50% of adults treated with phenytoin experience gingival enlargement, thirty% with cyclosporin, and 20% with nifedipine.[13]
Pathophysiology
In 1996, Seymour et al. postulated the theory of genetic predisposition for the etiopathology of DIGO.[three][fourteen] This is substantiated because some individuals develop gingival overgrowth and some exercise not whilst on the same drug. The usual inflammatory response of gingival fibroblasts and subsequent proliferation of connective tissue matrix emphasizes the heterogenetic character of the private'south gingival fibroblasts in response to the inducing drugs.
The common mechanism of action at the cellular level of all these three categories of dissimilar drugs appears to be inhibition of cation influx, especially sodium and calcium ions. Gingival overgrowth is multifactorial.[xiv][15][iv] Bacterial plaque appears to be a contributory cistron, and the severity of gingival overgrowth is straight proportional to the degree of plaque buildup and plaque-induced inflammation. Decreased cation dependant folic acid (FA) active ship within gingival fibroblasts causes reduced FA uptake by the cells, causing changes in the metabolism of matrix metalloproteinases and inability to activate collagenase. This results in an aggregating of connective tissue and collagen due to a lack of collagenase.
Gingival Fibroblasts and Cellular Folate Uptake
Inducing drugs act as a trigger for the activation and proliferation of gingival fibroblasts, causing an increased production of GAGs (glycosaminoglycans) in the connective tissue. These drugs decrease cellular uptake of folate by genetically predispose fibroblasts. Reduced intracellular folate translates into a decrease in the synthesis or activation of MMPs (matrix metalloproteinases), which are required to convert inactive collagenase to active collagenase, allowing an excess of connective tissue build up. Brown et al. (1991) postulated that bacterial plaque contributes to gingival inflammation, which completes the barbarous cycle.
Matrix M etalloproteinases
These are more 20 enzymes that bring nearly the degradation of connective tissue and tissue remodeling. These include collagenases, gelatinases, and stromelysins. Inhibition of activation of these can result in the accumulation of extracellular matrix and collagen and cause DIGO.
Inflammatory Cytokines
Inflamed gingival tissue exhibits higher levels of interleukin-1 beta (IL-1beta), a proinflammatory cytokine. Likewise, IL-6 causes fibroblastic proliferation and increased production of collagen and GAG synthesis.[4]
Na+/ Ca2+ ion Flux Drug Mechanisms
Fugi and Kobayashi (1990) reported inhibition of Ca2+ uptake within gingival fibroblasts past PHT and several calcium channel blockers (CCBAs). Thomas and Petrou (2013) reported a reduction in Na+ aqueduct availability and, therefore, a decrease in the action potential amplitude. This causes reduced Ca2+ entry, and a decrease in Ca2+ activated Yard+ channels. All three types of DIGO-inducing drugs human action on Ca2+ flux similarly.
Plaque Buildup
The concentrated drug in crevicular gingival fluid or bacterial plaque exerts a directly toxic consequence on the gingival tissue. Dental plaque induces inflammation, which causes gingival overgrowth. Inflammation causes the upregulation of transforming growth cistron-beta one (TGF-beta one). Hence, control of dental plaque is needed in the treatment and prevention of DIGO over time.
Histopathology
In DIGO, the pathological changes lie in the connective tissue and non the epithelial cells of the gingiva. In that location is an excessive accumulation of extracellular matrix-like collagen with varying amounts of inflammatory infiltrates, predominantly plasma cells. Fibroblastic proliferation may not be evident. Erratic columns of collagen fibers are seen interspersed with penetrating epithelial ridges.[4]
History and Physical
Patients with DIGO will study a past medical history of hypertension, angina, epilepsy, or contempo organ transplant. They typically present with gingival enlargement, hurting during mastication, and cosmetic disfigurement ane to 3 months afterward starting treatment with one of the drugs associated with the disease.[iv] The gingival enlargement caused past the drug makes oral hygiene challenging, leading to increased plaque aggregating, resulting in secondary inflammation.[16]
Not all drug-induced gingival overgrowth lesions are fibrotic similar it was previously believed. According to histological and histomorphometric analyses, phenytoin-induced lesions are the well-nigh fibrotic. Cyclosporin-induced lesions are more than inflamed and show a depression fibrotic component, and nifedipine lesions are mixed.[17]
Clinical Findings
-
Firm, painless, nodular enlargement of the interdental papilla, limited to the keratinized portions of the gingiva and extending to the facial and lingual gingival margins.
-
In severe cases, a huge fold of hypertrophied gingival tissue is observed covering the crowns.
-
If no secondary inflammation is present, it appears firm and pale pink with minute lobulations, pouting from underneath the gingival margin, delineated by a groove of tissue that does not bleed on affect.
-
If secondary inflammation exists, the gingiva appears smooth, and red or bluish-red.
-
The enlargement is generalized, simply it is commonly greater in the anterior regions.
-
Typically, it is not seen in edentulous areas.[16]
-
The gingival overgrowth disappears when teeth are extracted.[16]
Evaluation
The diagnosis of drug-induced gingival overgrowth is made by clinical exam and the patient's past medical history.
-
A periodontal examination is necessary to evaluate for the presence of periodontal disease.
-
Total mouth periapical radiographs and orthopantomography are required before kickoff any handling to dominion out periodontal disease.
-
Consummate claret count (CBC) is indicated in patients with gingival enlargement if there is a presence of profuse gingival bleeding, fifty-fifty if it is drug-induced, to rule out anemia and leukemia.
-
Tissue biopsy should exist carried out in example the presentation of the affliction is unusual.
-
Histopathological examination of persisting overgrowths is mandatory to evaluate malignant changes [12]
-
Candidiasis and other infections may exist ruled out past taking a civilization.
Treatment / Direction
The aim of handling in DIGO is to convalesce the patients' discomfort, enabling them to do elementary acts like eating and chewing hurting-gratuitous, treat the inflammation, reduce the swelling, and give a amend cosmetic appearance to the gingiva.
The modalities of handling are medical and surgical. Medical management is the beginning line of therapy, whereas surgery is reserved for recurrences or cases that persist despite expert medical handling.
Discontinuing or changing the medication must be placed under consideration.[18][13] An alternative to phenytoin includes carbamazepine and valproic acid, which accept shown a lower rate of gingival enlargement. Diltiazem and verapamil exhibit a lower prevalence of gingival enlargement compared to nifedipine. Cyclosporin substitution is more complicated considering at that place are express options available. Cyclosporin can be substituted by tacrolimus, and the use of azithromycin in combination with cyclosporin has shown a subtract in the severity of DIGO.[19]
Plaque control should be the first step in the treatment of DIGO, correct oral hygiene, and professional person plaque removal, including tooth surface cleaning and periodic scaling.[xx][21]
Control of inflammation, including non-steroidal anti-inflammatory agents, antibiotics to control infection, and topical antifungal medication like nystatin, may too be utilized. Folate supplementation has as well been used.[22]
A sufficient catamenia of six to twelve months should be allowed to expire after discontinuing the inducing drug before surgery is considered.[nineteen]The surgical methods include gingivectomy and periodontal flap surgery. Electrocautery may exist used in difficult cases, children, or where the gingiva is frail and probable to bleed. The CO2 laser has a wavelength of 10600 nm; hence, information technology is readily absorbed by water and is effective in the surgery of soft tissues with high h2o content like the gingiva. Claret vessels up to a diameter of 0.v mm can be sealed effectively and provide a dry field for better visibility of the surgical field. A laser is preferred over the scalpel as it has strong bactericidal and hemostatic effects.[20][ii]
The Function of Azithromycin in Cyclosporin Induced Gingival Overgrowth
In the last decade, researchers accept establish that azithromycin can help to reverse gingival overgrowth acquired by cyclosporine A in renal transplant patients.[23] Interestingly, azithromycin does not change the cyclosporin A blood levels or the renal function, avoiding the need of changing this drug to another anticonvulsant due to DIGO.[23]
The effect of azithromycin on cyclosporine A-induced collagen turnover and cell proliferation was studied by Kim et al. They ended that azithromycin: inhibits the proliferation of human gingival fibroblasts, and collagen aggregating - both induced past cyclosporin A – activates MMP-ii in renal transplant and normal fibroblast, inhibits mRNA levels of type 1 collagen and rises levels of MMP-2.[23]
Differential Diagnosis
-
False enlargement of gingival tissue: pseudo-enlargement of the gingiva, caused by an enlarged underlying bony tissue. The gingiva here has no aberration.
-
Inflammation: chronically inflamed gingival tissue is ruddy or violaceous, smooth, and tends to bleed on the touch.
-
Familial or hereditary conditions: examples include familial fibromatosis, idiopathic fibromatosis, gingivomatosis, and hereditary gingival hyperplasia. The gingiva is pink, non-tender, involves the fastened gingiva, the gingival margin, and the interdental papillae, and has a firm and leathery consistency.
-
Physiological states: puberty and pregnancy are associated with gingival enlargement.
-
Scurvy: vitamin C deficiency can produce very tender bleeding gingiva.
-
Systemic diseases: leukemia, tuberculosis, sarcoidosis - their diagnosis can be corroborated hematologically.
A thorough history, physical examination, and investigations, including biopsy, may be required to confirm the etiology in all these conditions.
Conditions Similar to Gingival Enlargement
-
Gristly epulis/peripheral fibroma
-
Angiogranuloma/Pyogenic granuloma
-
Gingival cysts
-
Neoplasms: They can be beneficial or malignant. Benign lesions include fibroma, peripheral and primal giant jail cell granuloma, papilloma, leukoplakia, nevus, hemangioma, leukoplakia, nevus, myoblastoma, hemangioma, neurilemoma, neurofibroma, ameloblastoma. Malignant tumors include squamous cell carcinoma, Kaposi'south sarcoma, among others.[24]
Prognosis
If the medication inducing the gingival overgrowth can be inverse to a drug that is less associated with this complication, the gingival tissue may return to normal with the aid of adequate plaque control. The gingival enlargement can persist, despite drug substitution and adept plaque control, and in this example, surgical management to restore normal gingival contours is required. These modalities of treatment, although constructive, do not always prevent the recurrence of the enlargement. DIGO recurrence in surgically treated cases may appear as soon as three to six months after the procedure. In general, the results terminal for at least twelve months.[2]
Complications
-
Functional difficulties
-
Esthetic concerns
-
Increased incidence of caries
-
Delayed eruption of teeth
-
Pathological drifting of teeth
-
Prolonged retention of the primary dentition
-
Diastemas and spacing problems
-
Poor plaque control leading to periodontal complications [two]
Deterrence and Patient Teaching
Some studies point that bacterial plaque is a prerequisite for the disease to occur. On the reverse, others believe that the presence of dental plaque is a result of the difficulty that the gingival enlargement represents to dental hygiene, which then exacerbates the severity of the overgrowth.[2] In whatsoever case, i affair is certain: bacterial plaque plays an essential role in developing DIGO, and patients must be educated near adequate dental brushing and flossing techniques that may exist accompanied by chlorhexidine gluconate rinses to control the levels of bacterial plaque. Regular appointments with their dentist must be achieved to perform professional cleaning of the teeth. These measures can forestall or decrease the rate and the degree to which recurrence occurs.
Enhancing Healthcare Team Outcomes
Since the status is entirely drug-induced, patient educational activity about the side furnishings of the implicated drugs before starting treatment is warranted, and the importance of good dental hygiene should be emphasized [two]. Drug-induced gingival enlargement has a adept prognosis and is generally reversible on stopping or substituting the offending drug. An interdisciplinary approach is needed as the principal clinician, the dentist, and the healthcare team should work together to address the patient'due south signs and symptoms adequately [Level V].
Review Questions
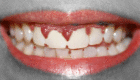
Figure
gingival overgrowth from a medication. Epitome courtesy S Bhimji Medico
![Gingival, [SATA]](https://www.ncbi.nlm.nih.gov/books/NBK538518/bin/gingival.gif)
Figure
Gingival, [SATA]. Contributed past Steve Bhmji, MS, MD, PhD
References
- 1.
-
Marshall RI, Bartold PM. Medication induced gingival overgrowth. Oral Dis. 1998 Jun;4(2):130-51. [PubMed: 9680902]
- 2.
-
Camargo PM, Melnick PR, Pirih FQ, Lagos R, Takei HH. Treatment of drug-induced gingival enlargement: artful and functional considerations. Periodontol 2000. 2001;27:131-viii. [PubMed: 11551304]
- iii.
-
Seymour RA, Thomason JM, Ellis JS. The pathogenesis of drug-induced gingival overgrowth. J Clin Periodontol. 1996 Mar;23(3 Pt i):165-75. [PubMed: 8707974]
- 4.
-
Dongari-Bagtzoglou A., Research, Science and Therapy Committee, American University of Periodontology. Drug-associated gingival enlargement. J Periodontol. 2004 Oct;75(10):1424-31. [PubMed: 15562922]
- 5.
-
Greenberg KV, Armitage GC, Shiboski CH. Gingival enlargement amid renal transplant recipients in the era of new-generation immunosuppressants. J Periodontol. 2008 Mar;79(3):453-60. [PubMed: 18315427]
- vi.
-
Sekiguchi RT, Paixão CG, Saraiva Fifty, Romito GA, Pannuti CM, Lotufo RF. Incidence of tacrolimus-induced gingival overgrowth in the absence of calcium aqueduct blockers: a brusque-term study. J Clin Periodontol. 2007 Jul;34(seven):545-50. [PubMed: 17433046]
- 7.
-
Nassar CA, Nassar PO, Andia DC, Guimarães MR, Spolidorio LC. The furnishings of up to 240 days of tacrolimus therapy on the gingival tissues of rats--a morphological evaluation. Oral Dis. 2008 Jan;14(1):67-72. [PubMed: 18173451]
- viii.
-
Cota LO, Oliveira AP, Costa JE, Cortelli SC, Costa FO. Gingival status of Brazilian renal transplant recipients under sirolimus-based regimens. J Periodontol. 2008 Nov;79(eleven):2060-eight. [PubMed: 18980514]
- 9.
-
Cota LO, Aquino DR, Franco GC, Cortelli JR, Cortelli SC, Costa FO. Gingival overgrowth in subjects under immunosuppressive regimens based on cyclosporine, tacrolimus, or sirolimus. J Clin Periodontol. 2010 October;37(10):894-902. [PubMed: 20618547]
- 10.
-
Cota LO, Viana MB, Moreira PR, Gomez RS, Cortelli JR, Cortelli SC, Costa FO. Gingival overgrowth in cyclosporine, tacrolimus, or sirolimus-based immunosuppressive regimens and the single nucleotide IL-6 (-174 G/C) gene polymorphism. Curvation Oral Biol. 2010 Jul;55(7):494-501. [PubMed: 20430366]
- 11.
-
Lafzi A, Farahani RM, Shoja MA. Amlodipine-induced gingival hyperplasia. Med Oral Patol Oral Cir Bucal. 2006 Nov 01;11(6):E480-2. [PubMed: 17072250]
- 12.
-
Samudrala P, Chava VK, Chandana TS, Suresh R. Drug-induced gingival overgrowth: A disquisitional insight into case reports from over two decades. J Indian Soc Periodontol. 2016 Sep-October;twenty(5):496-502. [PMC free article: PMC5676330] [PubMed: 29242684]
- 13.
-
Doufexi A, Mina Yard, Ioannidou Due east. Gingival overgrowth in children: epidemiology, pathogenesis, and complications. A literature review. J Periodontol. 2005 January;76(1):iii-ten. [PubMed: 15830631]
- fourteen.
-
Seymour RA, Ellis JS, Thomason JM. Risk factors for drug-induced gingival overgrowth. J Clin Periodontol. 2000 Apr;27(iv):217-23. [PubMed: 10783833]
- xv.
-
Dongari A, McDonnell HT, Langlais RP. Drug-induced gingival overgrowth. Oral Surg Oral Med Oral Pathol. 1993 Oct;76(4):543-8. [PubMed: 8233439]
- 16.
-
Bharti 5, Bansal C. Drug-induced gingival overgrowth: The nemesis of gingiva unravelled. J Indian Soc Periodontol. 2013 Mar;17(two):182-7. [PMC costless commodity: PMC3713748] [PubMed: 23869123]
- 17.
-
Trackman PC, Kantarci A. Molecular and clinical aspects of drug-induced gingival overgrowth. J Paring Res. 2015 Apr;94(4):540-6. [PMC free commodity: PMC4485217] [PubMed: 25680368]
- eighteen.
-
de la Rosa García Eastward, Mondragón Padilla A. [The effect of mycophenolate mofetil and azathioprine on gingival enlargement associated with cyclosporin A use in kidney transplant patients]. Nefrologia. 2009;29(5):474-8. [PubMed: 19820760]
- xix.
-
Diesel fuel A, Moriello K. Medical Management of Cyclosporine-Induced Gingival Overgrowth Using Oral Azithromycin in Half dozen Dogs. Vet Sci. 2015 Feb 05;two(i):xiii-22. [PMC complimentary article: PMC5644608] [PubMed: 29061926]
- 20.
-
Mavrogiannis M, Ellis JS, Thomason JM, Seymour RA. The management of drug-induced gingival overgrowth. J Clin Periodontol. 2006 Jun;33(vi):434-9. [PubMed: 16677333]
- 21.
-
Dhale RP, Phadnaik MB. Conservative management of amlodipine influenced gingival enlargement. J Indian Soc Periodontol. 2009 January;13(1):41-3. [PMC free article: PMC2846674] [PubMed: 20376240]
- 22.
-
Lu HK, Tseng CC, Lee YH, Li CL, Wang LF. Flutamide inhibits nifedipine- and interleukin-i beta-induced collagen overproduction in gingival fibroblasts. J Periodontal Res. 2010 Aug;45(iv):451-7. [PubMed: 20337887]
- 23.
-
Kim JY, Park SH, Cho KS, Kim HJ, Lee CK, Park KK, Choi SH, Chung WY. Mechanism of azithromycin treatment on gingival overgrowth. J Paring Res. 2008 November;87(xi):1075-9. [PubMed: 18946018]
- 24.
-
Agrawal AA. Gingival enlargements: Differential diagnosis and review of literature. Globe J Clin Cases. 2015 Sep 16;3(9):779-88. [PMC free article: PMC4568527] [PubMed: 26380825]
Source: https://www.ncbi.nlm.nih.gov/books/NBK538518/
0 Response to "Drug-induced Gingival Hyperplasia and Its Management a Literature Review"
Post a Comment